MacArthur’s Population and Reproductive Health program supported a critical paradigm shift from population control to women’s rights in the 1990s and contributed to decreases in maternal mortality rates through the 2000s. Today in Mexico, we are supporting another significant shift in reproductive health and rights by elevating the midwifery model of care.
Midwifery is low-intervention, low-cost, and evidence-based. It responds to women’s and infants’ needs, respects cultural identities, and embodies dignity and respect. And midwifery has the capacity to support women’s access to reproductive care, ensure control over their reproductive choices, and reduce maternal mortality.
When we began our midwifery initiative in 2015, we were responding to Mexico’s failure to reach the UN’s Millennium Development Goal of reducing maternal mortality by 75 percent. Mexico was unable to achieve that goal, in part, because too many deliveries were channeled to the hospital system; hospitals were overburdened with routine, normal deliveries; and the medical system lost capacity for more urgent cases and other primary care services. Impacts included a lack of access to quality care, overuse of medical interventions, increasing rates of teen pregnancy, obstetric violence, and the world’s third highest cesarean section rate.
Growing frustration with the medicalization of birth made civil society organizations keen to focus on a solution. Yet there was little awareness of professional midwifery, and there was no official information available. Our 2015 baseline research found only 174 “midwives” in the public health system. In general, people were familiar with traditional, indigenous, rural, or self-taught midwifery, but the idea of university-level midwifery was foreign, stigmatized, and largely misunderstood.
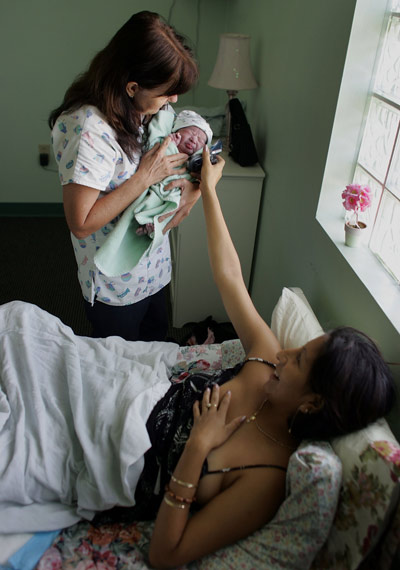
© Getty Images
Our initiative’s theory of change posited that if Mexico could deploy competent professional midwives in healthcare facilities, then over time the quality of care would improve, maternal mortality would decrease, and access to reproductive healthcare would expand. There would also be greater equity for marginalized and vulnerable communities and better programmatic and financial efficiency in the healthcare system.
Since 2015, we have invested over $17 million in 35 organizations—from grassroots groups to multilateral agencies—that together have made significant progress in growing public acceptance, opening new training programs, and improving midwifery service delivery. Their collective work seeks to take the country to a tipping point at which reproductive health planners and practitioners can no longer ignore the fact that midwifery is an essential but missing piece of the healthcare system.
First, we sought to build momentum through strengthening networks and leadership and promoting legitimacy and demand. Our forthcoming progress report shows that support of midwifery increased and that discourse began to change.
There is new leadership from ministries of health, universities, practitioners, and civil society at the state and federal levels. Fourteen of 32 state health ministries have taken on the midwifery banner. Four states have intersectoral working groups to promote midwifery that include the state education, population, and health authorities along with local organizations and midwives. People in influential positions draw on information our grantees developed to advocate for better care through midwifery—for example, research by the National Institute of Public Health shows that deliveries by midwives in Mexico cost almost half what they cost when done by doctors.
Advances in education have nearly doubled the number of accredited midwifery training programs since 2015—from seven to twelve—with at least three others poised to open in 2019. Enrollment increased from 650 to 2,150 students annually. Hundreds of seminars, workshops, meetings, and a basic online course have reached more than 6,000 health authorities and practitioners.
The program also seeks to place midwives in effective employment. In 2017, a $1 million grant to the Pan American Health Organization supported a competition for state-level Ministries of Health already working with the midwifery model, thereby directly engaging and empowering operators. The Ministry of Health announced the competition at a meeting with all 32 state health ministries; it received 17 projects and selected 10 for enhanced training, equipment, and salaries. The 36 deployment sites present in 2018 are complying better with the standards of the midwifery model of care than the 19 there were in 2015.

No other country in the world has experienced the growth of midwifery opportunities that Mexico has in these past three years. Even so, challenges remain in ensuring stable and quality integration of midwives into healthcare teams, such as budget cuts, short-term employment contracts, and complicated dynamics of clinic-level teamwork.
Midwifery advocates seek to enlarge their community of supporters and develop a more unified voice and strategy. Despite impressive gains in a short period of time, legitimacy, understanding, and support are still uneven. Even where midwives are working, administrative loopholes keep them from fully exercising their profession. They are overqualified, underpaid, and vulnerable to budget cuts. They are subject to gender, cultural, and labor discrimination.
Momentum toward this paradigm shift is stronger than ever. State leaders say to ensure continuity they seek a federal mandate, inclusion in the National Development and Health Plans, and support in federal and state budgets. Midwifery can help reduce public spending and out-of-pocket costs for women and their families.
We are privileged to support the many advocates from women’s health and rights organizations, national and state health authorities and service providers, multilateral agencies, midwifery students, and midwives themselves as they forge the path toward universal access to high-quality reproductive health services for all women in Mexico.



